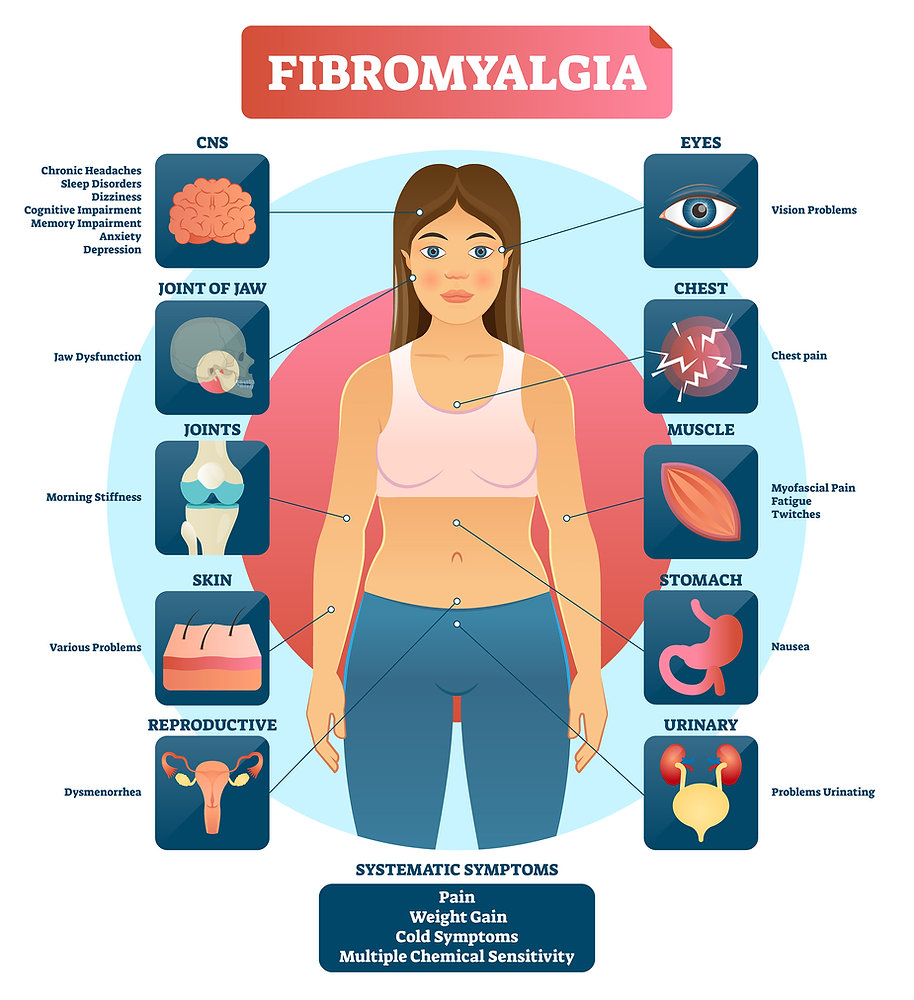
Fibromyalgia is a chronic condition that involves symptoms such as muscle and joint pain, fatigue, sleep problems, and mental stress. The condition is primarily associated with abnormal sensitivity (hypersensitivity) of the nervous system. Electrical nerve stimulation (ENS) therapy can help this condition in the following ways:
1. Controlling pain sensitivity
ENS therapy blocks or modulates the pain signals of the nervous system. It works under the “gate control theory”, where pain signals are blocked before they reach the brain by sending mild electrical impulses. This can reduce fibromyalgia pain.
2. Improving neurochemical balance
ENS therapy can improve the levels of neurotransmitters (such as serotonin and dopamine), which play an important role in mood and pain control. This helps reduce mental stress and depression often seen in fibromyalgia.
3. Improve sleep and fatigue
Fibromyalgia patients experience fatigue due to lack of deep sleep. ENS therapy calms the neural activity in the brain, which can improve sleep quality. This reduces fatigue and increases the patient’s energy level.
4. Reduce muscle and tissue inflammation
ENS therapy reduces muscle inflammation and stiffness by increasing blood flow to the affected area. This helps reduce muscle pain and increase their flexibility.
5. “Reset” the nervous system
The central nervous system is more sensitive in fibromyalgia. ENS therapy can work to balance the nervous system and “reset” it, thereby controlling the patient’s symptoms in the long term.
Curing Fibromyalgia using Neurotherapy, Neurostimulation Therapy, Neuromodulation Therapy, Neurobiomarker Therapy, and Synthetic Stem Cell Therapy is scientifically plausible because these approaches address the underlying mechanisms of the condition. Fibromyalgia is characterized by chronic widespread pain, fatigue, and cognitive dysfunction (often referred to as “fibro fog”). These therapies aim to restore neural and physiological balance, targeting pain processing, inflammation, and cellular repair.
1. Neurotherapy: Neurotherapy focuses on retraining the brain to modulate pain perception and enhance neural pathways involved in relaxation and resilience.
Mechanism:
Pain Perception Regulation: Neurotherapy helps the brain recalibrate overactive pain pathways by targeting areas like the anterior cingulate cortex and prefrontal cortex.
Stress and Fatigue Reduction: Chronic stress exacerbates fibromyalgia symptoms. Neurotherapy improves autonomic nervous system (ANS) regulation, reducing sympathetic overdrive.
Scientific Basis: Studies show that neurofeedback and biofeedback can modulate brainwave patterns, reducing pain sensitivity and improving sleep quality in fibromyalgia patients. Improved ANS balance lowers systemic inflammation and reduces muscle tension, alleviating widespread pain.
2. Neurostimulation Therapy: Techniques like Transcranial Magnetic Stimulation (TMS), Transcutaneous Electrical Nerve Stimulation (TENS), and Vagus Nerve Stimulation (VNS) can directly modulate neural circuits involved in pain and fatigue.
Mechanism:
TMS: Targets the motor cortex and prefrontal cortex to recalibrate abnormal pain processing.
TENS: Reduces localized muscle pain and improves blood flow to affected areas.
VNS: Enhances parasympathetic activity, reducing inflammation and promoting relaxation.
Scientific Basis: Clinical trials show TMS significantly reduces pain and improves mood in fibromyalgia patients by altering cortical excitability. VNS has been shown to reduce systemic inflammation, which is often elevated in fibromyalgia.
3. Neuromodulation Therapy: Neuromodulation involves targeted electrical or magnetic interventions to normalize neural activity and improve communication between the brain and body.
Mechanism:
Spinal Cord Stimulation (SCS): Modulates pain signals at the spinal level, reducing their transmission to the brain.
Closed-loop Neuromodulation: Adapts stimulation based on real-time feedback from the nervous system, optimizing pain relief.
Scientific Basis: SCS is already used to treat chronic pain conditions, with studies showing significant pain reduction in fibromyalgia patients. Neuromodulation improves connectivity in neural networks involved in pain processing and emotional regulation.
4. Neurobiomarker Therapy: Identifying and targeting specific biomarkers in fibromyalgia allows for precise treatment tailored to the individual’s condition.
Mechanism:
Inflammatory Biomarkers: Chronic low-grade inflammation, indicated by cytokines like IL-6 and TNF-α, can be monitored and reduced.
Neurochemical Imbalances: Dysregulation of neurotransmitters such as serotonin, dopamine, and norepinephrine can be corrected.
Autonomic Biomarkers: Assessing heart rate variability (HRV) can help in managing ANS dysfunction.
Scientific Basis: Biomarker-based interventions ensure early diagnosis and monitoring of treatment response. Reducing inflammation and balancing neurotransmitters improves pain perception, mood, and energy levels.
5. Synthetic Stem Cell Therapy: Synthetic stem cells have the potential to repair damaged tissues and restore normal neural and muscular function in fibromyalgia.
Mechanism:
Neural Repair: Stem cells can repair damaged neural pathways involved in pain processing.
Muscle Recovery: Stem cells can regenerate muscle tissues affected by chronic tension and fatigue.
Anti-inflammatory Effects: Stem cells reduce systemic inflammation, alleviating symptoms like pain and stiffness.
Scientific Basis: Research shows that stem cell therapy can reduce inflammation and promote neural regeneration, addressing key aspects of fibromyalgia pathology. Synthetic stem cells are engineered for targeted delivery, enhancing their efficacy and minimizing side effects.
Why a Complete Cure is Theoretically Possible:
1. Targeting Pain Processing: Neurostimulation and neuromodulation therapies recalibrate overactive pain pathways in the central nervous system (CNS). This reduces hyperalgesia (increased pain sensitivity) and central sensitization, hallmarks of fibromyalgia.
2. Reversing Neural and Muscular Dysfunction: Stem cells repair neural pathways and regenerate damaged muscle tissues, addressing the physical manifestations of fibromyalgia.
3. Correcting Systemic Imbalances: Neurotherapy and neurobiomarker-guided treatments address the dysregulation of neurotransmitters, inflammation, and ANS function.
4. Personalized and Integrated Approach: Combining these therapies ensures all aspects of the condition—pain, fatigue, cognitive dysfunction, and inflammation—are addressed simultaneously.
Limitations and Challenges:
Chronic Nature: Fibromyalgia is a chronic condition influenced by genetic, environmental, and lifestyle factors, requiring a holistic approach.
Accessibility and Cost: Advanced treatments like synthetic stem cells and neuromodulation devices are expensive and not yet widely available.
Research and Validation: These therapies are still under investigation for fibromyalgia, and more clinical trials are needed to confirm their long-term efficacy.
Summary: The combination of neurotherapy, neurostimulation, neuromodulation, neurobiomarker therapy, and synthetic stem cell therapy offers a comprehensive solution to curing fibromyalgia. These therapies address the root causes, including central sensitization, inflammation, and neural dysfunction. While further research and clinical validation are needed, these approaches hold significant promise for achieving a complete cure for fibromyalgia.