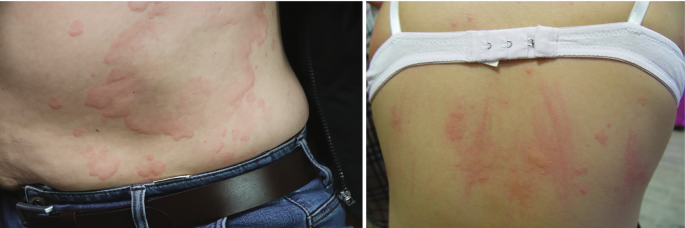
tVNS (Transcutaneous Vagus Nerve Stimulation) can be helpful in managing and treating allergies. This technique is effective in controlling the body’s immune response and reducing inflammation.
Relation between tVNS therapy and allergies
1. Immune System Modulation: Allergies occur when the body’s immune system overreacts to normal substances (such as dust, pollen, or food) mistaking them for harmful substances. tVNS therapy stabilizes the immune system by stimulating the vagus nerve and helps it function normally.
2. Regulating Cytokines: During allergies, the level of cytokines (inflammation-inducing proteins) increases in the body. tVNS therapy reduces these cytokines and prevents inflammation and allergic reactions.
3. Balancing the Autonomic Nervous System: tVNS reduces stress by activating the parasympathetic nervous system. Stress can also aggravate allergy symptoms, and its control helps in treating allergies.
4. Reducing Inflammation: Allergies often cause inflammation in the respiratory tract or skin. tVNS therapy is helpful in reducing inflammation, gradually reducing allergy symptoms.
5. Improved Brain-Body Communication: The vagus nerve is the main link between the brain and the body. tVNS improves this connection, thereby reducing the body’s allergic response.
Completely curing allergies with a combination of neurotherapy, neurostimulation therapy, neuromodulation therapy, neurobiomarker therapy, and synthetic stem cell therapy is a fascinating proposition. Allergies result from an overactive immune response to harmless substances (allergens), often mediated by the nervous and immune systems. These advanced approaches could theoretically target the root causes of allergies at both the cellular and systemic levels. Here’s how each method could contribute and the scientific reasoning behind it:
1. Neurotherapy
How It Helps: Neurotherapy focuses on rebalancing the autonomic nervous system (ANS) and modulating the brain’s response to allergic triggers. Techniques like neurofeedback and biofeedback can reduce stress and hypersensitivity, which often exacerbate allergic reactions.
Scientific Basis: Allergies are influenced by the ANS, particularly the parasympathetic branch. An overactive sympathetic response can worsen inflammation and immune overreaction. By training the brain to regulate these responses, neurotherapy could lower the body’s hypersensitivity to allergens over time.
2. Neurostimulation Therapy
How It Helps: Neurostimulation, such as transcranial magnetic stimulation (TMS) or transcutaneous electrical nerve stimulation (TENS), can alter neural circuits involved in inflammation and immune regulation.
Scientific Basis:
Vagus nerve stimulation (VNS): The vagus nerve plays a critical role in the inflammatory reflex, which controls systemic inflammation.
VNS has been shown to: Reduce the release of inflammatory cytokines (e.g., IL-4, IL-5, IL-13) responsible for allergic responses. Improve immune system tolerance to allergens. This approach could reduce the severity and frequency of allergic reactions.
3. Neuromodulation Therapy
How It Helps: Neuromodulation involves altering neural pathways to regulate immune system activity and reduce hypersensitivity to allergens.
Scientific Basis: The nervous system and immune system are tightly interconnected. Neuromodulation can: Decrease mast cell activation, a key driver of allergic reactions (e.g., histamine release). Enhance regulatory T-cell (Treg) function, which suppresses the overactive immune response seen in allergies. Targeted neuromodulation (e.g., through VNS or spinal cord stimulation) can lead to long-term immune tolerance to allergens.
4. Neurobiomarker Therapy
How It Helps: Neurobiomarker therapy involves identifying specific biomarkers (molecular or neural) associated with allergic reactions and tailoring treatments accordingly.
Scientific Basis:
A. Biomarker Identification: Allergies are associated with biomarkers such as: IgE antibodies (specific to allergens). Eosinophils and related cytokines (e.g., IL-5). Neuropeptides (e.g., substance P) that amplify immune responses. Neurobiomarkers related to the ANS (e.g., heart rate variability) can indicate autonomic dysregulation in allergy sufferers.
B. Targeted Therapy: Using biomarkers, neuromodulation and neurostimulation therapies can be customized for individuals, ensuring precise and effective treatment.
5. Synthetic Stem Cell Therapy
How It Helps: Synthetic stem cells can repair damaged tissues, restore immune balance, and create immune tolerance to allergens.
Scientific Basis:
A. Immune Modulation: Stem cells can suppress allergic inflammation by: Increasing Treg cells, which suppress the overactive immune response. Decreasing pro-inflammatory cytokines (e.g., IL-4, IL-13). Promoting a shift from a Th2-dominated response (allergy-prone) to a Th1-dominated response (normal immune function).
B. Tissue Repair: Allergies, especially respiratory allergies, can damage tissues (e.g., airway epithelium). Synthetic stem cells can regenerate these tissues, restoring normal function.
C. Immune Tolerance: Synthetic stem cells can “educate” the immune system to tolerate allergens, potentially eliminating hypersensitivity permanently.
Mechanism of a Cure
By combining these therapies, it might be possible to cure allergies through a multi-pronged approach:
A. Immune Regulation: Neurotherapy, neuromodulation, and synthetic stem cells can collectively modulate immune responses, preventing overreaction to allergens.
B. Inflammation Reduction: Neurostimulation and neuromodulation suppress key inflammatory pathways and cytokines involved in allergic reactions.
C. Tissue Regeneration: Synthetic stem cell therapy repairs damage caused by chronic allergic inflammation, restoring tissue integrity and function.
D. Customized Precision Treatment: Neurobiomarkers allow for precise targeting of underlying mechanisms specific to each individual’s allergies.
E. Neural Rewiring: Neurotherapy and neuromodulation can retrain the nervous system to stop triggering allergic responses to harmless substances.
Challenges and Limitations
1. Complexity of Allergies: Allergies vary widely in their causes and manifestations (e.g., food, respiratory, skin). A universal cure may require personalization for different allergy types.
2. Long-term Efficacy: While these therapies show potential, long-term studies are needed to confirm their ability to permanently cure allergies.
3. Ethical and Safety Concerns: Synthetic stem cell therapy, though promising, must undergo rigorous testing to ensure safety and prevent adverse effects.
4. Cost and Accessibility: Combining advanced therapies like stem cells and neuromodulation may be expensive, limiting accessibility.
Conclusion
The combination of neurotherapy, neurostimulation, neuromodulation, neurobiomarker therapy, and synthetic stem cell therapy offers a scientifically plausible pathway to curing allergies. These methods address the underlying immune dysregulation, repair tissue damage, and retrain the nervous system, potentially eliminating the root causes of allergies. However, significant research, clinical trials, and technological advancements are needed to validate and implement this approach as a reliable cure.