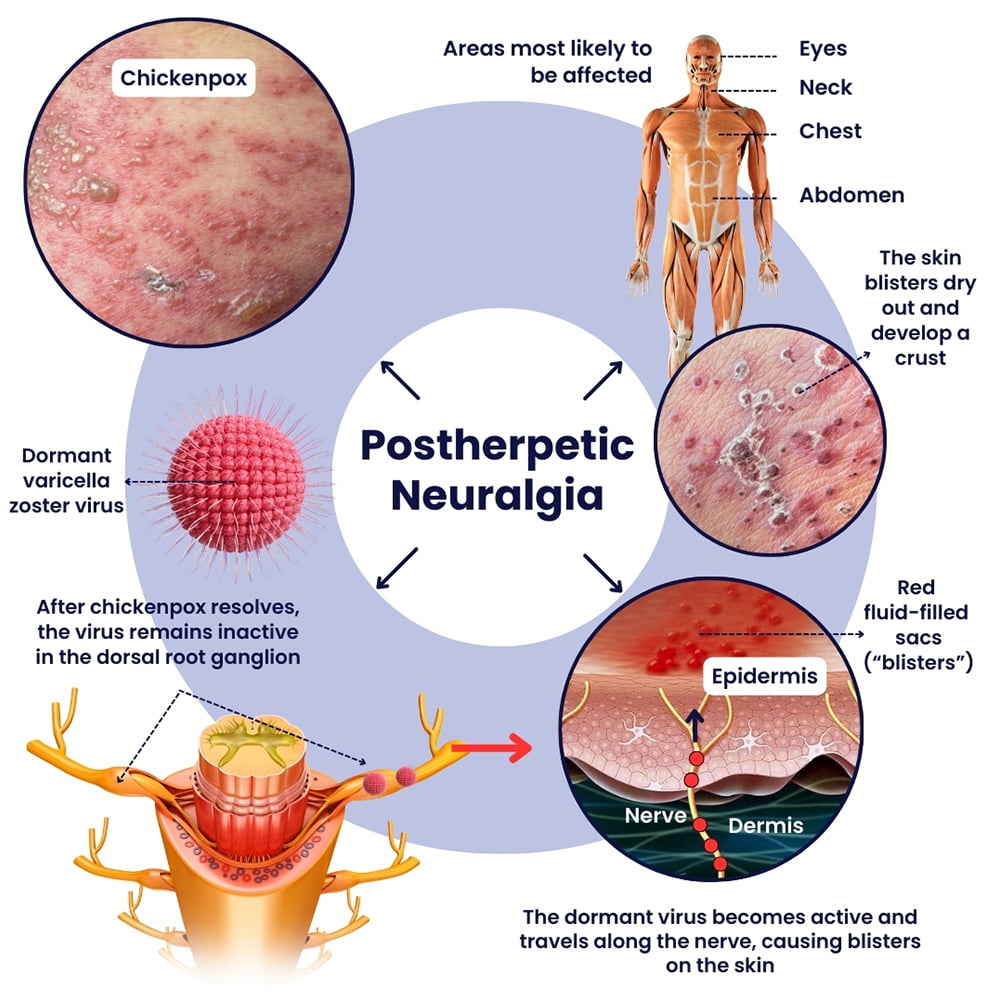
Post-herpetic neuralgia (PHN) is a condition that occurs after herpes zoster (shingles). It involves damage to the nerves, causing long-term pain, burning, numbness, or sensitivity. Electrical nerve stimulation (ENS) therapy can be effective in treating this condition.
1. Pain Signal Modulation:
ENS therapy sends mild electrical impulses to the nerves, which blocks the pain signals before they reach the brain. This provides immediate pain relief.
2. Nerve Healing:
In PHN, the nerves are damaged, making them overly sensitive. ENS therapy improves blood flow and nutrition to the damaged nerves, thereby speeding up nerve repair and reactivation.
3. Balancing the central nervous system:
In PHN, the brain and nervous system become overly sensitive, making even mild pain feel intense. ENS therapy balances the nervous system and reduces pain permanently.
4. Reducing inflammation and irritation:
Inflammation and irritation of the nerves are common in PHN. ENS therapy soothes the nerves by reducing inflammation and restores their normal function.
5. Rebuilding tissues and nerves:
ENS therapy helps reactivate tissues and nerves to restore them to their original state.
Curing Post-Herpetic Neuralgia (PHN) using Neurotherapy, Neurostimulation Therapy, Neuromodulation Therapy, Neurobiomarker Therapy, and Synthetic Stem Cell Therapy is theoretically possible by addressing the root causes of this condition. PHN, a chronic pain condition following shingles (herpes zoster), arises from nerve damage, inflammation, and abnormal pain signaling. These therapies can alleviate symptoms and repair damaged neural pathways.
1. Neurotherapy: Neurotherapy focuses on retraining the brain to reduce pain perception and improve nerve function.
Mechanism:
Pain Signal Recalibration: Neurofeedback trains the brain to reduce hyperactive pain signaling in regions such as the somatosensory cortex.
Stress and Pain Reduction: Biofeedback reduces stress, which exacerbates nerve pain, by promoting relaxation and parasympathetic activation.
Scientific Basis: Studies demonstrate that neurofeedback can modulate brain activity associated with chronic pain, helping to alleviate pain and improve quality of life. Stress management through neurotherapy decreases cortisol levels, reducing nerve inflammation and pain sensitivity.
2. Neurostimulation Therapy: Neurostimulation techniques like Transcutaneous Electrical Nerve Stimulation (TENS) and Transcranial Magnetic Stimulation (TMS) can directly target nerve dysfunction and pain in PHN.
Mechanism:
Pain Gate Control: TENS stimulates non-painful sensory pathways, inhibiting pain signals transmitted to the brain.
Neuroplasticity Enhancement: TMS promotes neural reorganization, reducing abnormal pain processing.
Peripheral Nerve Healing: TENS improves blood flow and reduces inflammation in the affected nerves.
Scientific Basis: Clinical trials have shown that TENS reduces neuropathic pain by activating the pain gate control mechanism. TMS has proven effective in modulating cortical excitability, reducing pain intensity in PHN patients.
3. Neuromodulation Therapy: Neuromodulation therapy uses targeted electrical stimulation to regulate neural circuits involved in chronic pain.
Mechanism:
Spinal Cord Stimulation (SCS): Modulates pain transmission in the dorsal column, reducing the intensity of pain signals from damaged nerves.
Vagus Nerve Stimulation (VNS): Activates anti-inflammatory pathways and reduces pain perception by stimulating the parasympathetic nervous system.
Closed-Loop Neuromodulation: Provides real-time adjustments to optimize pain relief based on feedback from the nervous system.
Scientific Basis: SCS has been widely used to treat neuropathic pain, including PHN, by disrupting pain signal transmission. VNS has demonstrated efficacy in reducing inflammation and chronic pain through its effects on the central and peripheral nervous systems.
4. Neurobiomarker Therapy: Using biomarkers to guide therapy enables targeted interventions for PHN by identifying and treating specific physiological abnormalities.
Mechanism:
Inflammatory Biomarkers: Identifies elevated cytokines like IL-6 and TNF-α, which contribute to nerve inflammation and pain.
Nerve Damage Markers: Tracks indicators of peripheral nerve injury, enabling precise monitoring of recovery.
Neurotransmitter Imbalances: Identifies deficits in GABA, serotonin, or dopamine, which can be corrected to improve pain modulation.
Scientific Basis: Biomarker-guided therapies allow for early intervention and precise monitoring of treatment effectiveness in reducing nerve inflammation and pain sensitivity. Targeting specific pathways of inflammation and neural damage has shown promise in neuropathic pain management.
5. Synthetic Stem Cell Therapy: Synthetic stem cell therapy has the potential to repair nerve damage and restore normal function in PHN.
Mechanism:
Nerve Regeneration: Stem cells promote the repair of damaged peripheral nerves by differentiating into neuronal or supportive glial cells.
Anti-inflammatory Effects: Stem cells release cytokines and growth factors that suppress inflammation and enhance tissue healing.
Neurotransmitter Restoration: Synthetic stem cells can restore the balance of pain-regulating neurotransmitters in the nervous system.
Scientific Basis: Studies have shown that mesenchymal stem cells (MSCs) reduce neuropathic pain by regenerating damaged nerves and suppressing inflammation. Synthetic stem cells, designed for targeted delivery, improve safety and efficacy in repairing nerve injuries without the risk of rejection.
Why a Complete Cure is Theoretically Possible:
1. Targeting Pain Processing Pathways: Neurostimulation and neuromodulation therapies disrupt abnormal pain signals and enhance neuroplasticity, reducing PHN symptoms.
2. Repairing Nerve Damage: Synthetic stem cell therapy regenerates damaged peripheral nerves, restoring their function and preventing recurrent pain.
3. Reducing Inflammation: Neurobiomarker therapy identifies and addresses chronic inflammation, a key driver of PHN pain, while stem cells enhance tissue healing.
4. Holistic Approach: Combining these therapies ensures comprehensive management of PHN by addressing pain, inflammation, nerve damage, and psychological factors.
Limitations and Challenges:
Chronic Nature of PHN: Long-standing nerve damage may require extended therapy durations for full recovery.
Cost and Accessibility: Advanced therapies like synthetic stem cells and neuromodulation are expensive and not widely available.
Research and Validation: While promising, these therapies require further clinical trials to establish their long-term efficacy and safety for PHN.
Summary: A complete cure for Post-Herpetic Neuralgia is theoretically possible with an integrated approach involving Neurotherapy, Neurostimulation Therapy, Neuromodulation Therapy, Neurobiomarker Therapy, and Synthetic Stem Cell Therapy. These therapies work together to address the root causes of PHN, including pain dysregulation, nerve damage, and inflammation, offering a scientifically grounded path to recovery. Further research and clinical advancements are necessary to make these treatments more accessible and effective.